Red light therapy knee pain: wavelengths, timing, and real results

Red light therapy knee pain relief usually comes down to three dials you can control at home: wavelength (red ~660nm and near-infrared ~850nm), dose (minutes per session), and consistency (sessions per week). In practice, most people do best with a combo of 660nm + 850nm, 10–15 minutes per side, 3–5 times weekly. And, you’ll typically need 2–4 weeks to notice meaningful changes in stiffness or post-activity soreness—sometimes sooner, sometimes not.
I’ve used light therapy on cranky knees after long walks and, honestly, the biggest mistake I see is people blasting a knee once and calling it “not working.” Instead, this is more like rehab than a painkiller. Therefore, if you’re going to try it, set a simple schedule, track symptoms, and treat it like a four-week experiment.
One more real-world note: if you’re already working on strength, sleep, and protein intake, you’ll usually notice light sessions more. For example, I’ve found my “after stairs” ache drops faster when I’m also consistent with basic quad and glute work. Also, if you’re low on nutrients (vitamin D, magnesium, etc.), a basic daily supplement can support recovery—just don’t expect it to replace the basics.
Below, I’ll break down what the research and clinical practice most consistently point to: the best-supported wavelengths, session length, weekly frequency, and how long results usually take for osteoarthritis and overuse pain.
what’s red light therapy for knee pain, and what does it actually do?
Red light therapy knee pain protocols use red (visible) and near-infrared (invisible) light to deliver a measured dose of energy to tissues around the knee. The goal is to support cellular energy production (ATP), reduce oxidative stress, and nudge inflammation in a friendlier direction. That’s why, many people report less stiffness, easier movement in the morning, and less “hot” soreness after activity.
To be clear, it’s not magic. It won’t “regrow cartilage” overnight. However, it may help symptoms and function—especially when paired with exercise and smart load management.
Evidence-wise, photobiomodulation has been studied for knee osteoarthritis and pain. A 2019 systematic review and meta-analysis in BMJ Open reported that certain wavelength-dose combinations were associated with reduced pain and improved function in knee OA, while dosing matters a lot (too low or too high can underperform). Source: BMJ Open (2019).
And, research from the CDC shows that about 12.5% of U.S. adults (18+) have arthritis-attributable activity limitation. Source: CDC arthritis statistics.
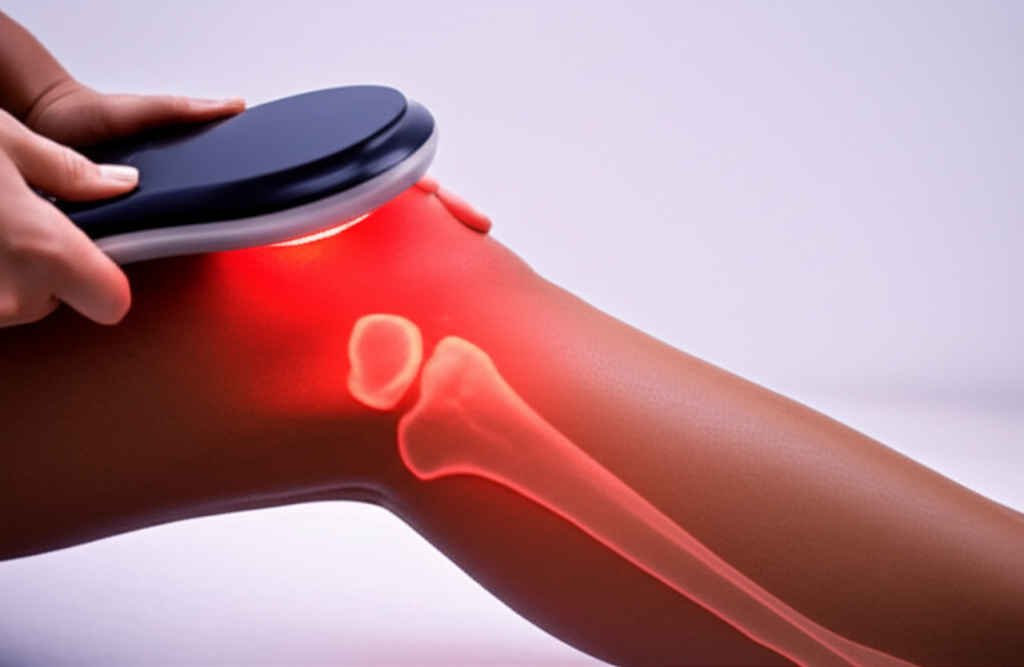
Which wavelengths work best: 660nm vs 850nm?
If you’re shopping, you’ll see the same numbers again and again. There’s a reason for that.
- 660nm (red): Often used for more superficial tissue targets (skin, superficial tendons, front-of-knee structures). Plus, many users find it helpful for “surface-level” ache and stiffness.
- 850nm (near-infrared): Penetrates deeper than red, so it’s typically favored for deeper joint structures and thicker tissue areas. Therefore, for knees—especially larger knees or deeper pain—850nm is a common staple.
In my experience, the best home devices for knees include both 660nm and 850nm. Why choose, if you don’t have to? A combo panel or targeted wrap that mixes wavelengths usually covers more bases. Still, if you only had one, I’d lean 850nm for knees because depth matters.
Interestingly, dosing guidelines in research often sit in the neighborhood of a few joules per point (not “as much as possible”). That’s why irradiance and time matter more than marketing claims.
How long should a session be for knee pain?
Most at-home knee sessions land in a sweet spot: 10–15 minutes per side, with the light positioned close enough to deliver a meaningful dose (often a few inches away, depending on device instructions). However, session length should be tied to irradiance (power density), not vibes.
Here’s a simple way to think about it:
- Higher irradiance device (stronger output): you need less time.
- Lower irradiance device (weaker output): you need more time—or you may never reach an effective dose.
For many consumer devices, 10 minutes is a reasonable start. Then, if you tolerate it well, you can move toward 12–15 minutes. More than that isn’t automatically better; in fact, photobiomodulation can be biphasic (too much may reduce benefits).
How often should you do it each week?
Consistency beats hero sessions. For these routines, most people do best with 3–5 sessions per week. Plus, if you’re flared up, you might do 5 days per week for two weeks, then back down to 3 days per week for maintenance. Still, it’s smart to keep a “minimum effective schedule” you can actually stick to.
For osteoarthritis, the pattern I see most often is:
- Weeks 1–2: 4–5 sessions/week
- Weeks 3–4: 3–4 sessions/week
- After that: 2–3 sessions/week as needed
Also, if you’re doing hard leg training or long hikes, placing sessions on the same day can be helpful. Meanwhile, some people prefer evenings because stiffness feels better the next morning.
When will you notice results (and what should change first)?
Most folks notice something in 2–4 weeks, assuming the device output is decent and the schedule is consistent. Occasionally, people feel a “looser” knee after the first few sessions. More often, the first changes are subtle.
What typically improves first:
- Morning stiffness (getting moving feels easier)
- Post-walk soreness (less ache later in the day)
- Range of motion comfort (stairs feel less cranky)
What takes longer:
- Swelling patterns (especially if your workload stays high)
- Big functional jumps (running, deep squats)
Notably, knee osteoarthritis is extremely common. The CDC estimates that around 32.5 million U.S. adults have osteoarthritis (all joints). Source: CDC osteoarthritis basics. That doesn’t prove this works, of course, but it’s why so many people are hunting for non-drug options.
Plus, a large 2019 Global Burden of Disease analysis reported that knee osteoarthritis accounted for about 60.6% of OA burden worldwide. Source: The Lancet Rheumatology (GBD/OA).
At-home device checklist: what I’d look for before buying
Buying a device is where people get burned. The box can say “medical-grade” and still be vague about output. Therefore, I use a short checklist.
- Wavelengths listed clearly: Look for 660nm and/or 850nm (or close neighbors like 630–670 and 810–850).
- Irradiance (mW/cm²) disclosed at a specific distance: If they won’t tell you output at 6 inches (or similar), that’s a red flag.
- Treatment area size: A tiny spotlight can work, but you’ll spend forever covering the whole knee. Therefore, a medium panel or flexible wrap is often more practical.
- Timer and consistent positioning: Built-in timers keep dosing consistent. Also, stable stands help you avoid constantly changing distance.
- Cooling/comfort: Some panels get warm. Mild warmth is fine, but you don’t want heat driving symptoms.
- Eye safety guidance: Red light is bright. NIR is invisible. Follow the manufacturer’s eye protection advice and don’t stare into LEDs.
- Return policy and warranty: Your knee won’t care about hype, but your wallet will.
If you want a quick add-on that supports joint recovery in a boring-but-useful way, I’ve seen people do well pairing their knee plan with a basic protein routine and a simple Amazon-sourced daily vitamin (nothing fancy). It’s not a “knee cure,” yet it can cover gaps when life gets messy. For more on evidence-based OA self-management, you can also check guidance from NIAMS (NIH).
Simple 4-week protocol you can actually follow
This is the exact structure I’d give a friend who says, “Just tell me what to do.” It’s simple on purpose. On top of that, it includes a built-in way to tell if it’s helping.
Before you start (5 minutes, once)
- Pick one main metric: morning stiffness (0–10) or pain on stairs (0–10).
- Pick one function test: time for a comfortable 10-minute walk, or how many sit-to-stands feel okay.
- Write down your baseline. Seriously—memory lies.
Weeks 1–2 (build consistency)
- Frequency: 5 days/week
- Time: 10 minutes per side
- Position: Front/medial knee one day, then rotate angles slightly to cover the joint line
Weeks 3–4 (optimize)
- Frequency: 3–4 days/week
- Time: 12–15 minutes per side (only if weeks 1–2 felt fine)
- Add-on: Gentle quad work 2–3 days/week (for example, wall sits or straight-leg raises)
Meanwhile, keep your normal activity steady. Otherwise, don’t suddenly add hill sprints and then blame the light when your knee complains.
Precautions, red flags, and when to see a clinician
Most people tolerate light therapy well. Still, you should use common sense.
- Stop and reassess if pain clearly worsens over several sessions.
- Avoid shining directly into eyes. Use provided goggles if recommended.
- Be careful with heat: if the device warms your skin, increase distance or shorten time.
- Medication note: If you’re on photosensitizing meds, ask your clinician first.
See a clinician sooner (not later) if you’ve:
- locking, true giving-way, or a sudden loss of range of motion
- significant swelling after minor activity
- fever, redness, or warmth suggesting infection
- pain after an acute injury (twist/pop) that doesn’t settle
Also, if you suspect osteoarthritis but haven’t had a proper assessment, a physical therapist can be a cheat code. Then you’ll get a plan that targets the real drivers (strength, mobility, load), and the light becomes a “support tool” rather than the whole strategy. If you want a starting point on what PT often targets for knee OA, see APTA clinical practice guidelines.
Does red light therapy help osteoarthritis, overuse pain, or both?
In my opinion, it’s most useful for two buckets:
- Osteoarthritis symptoms (stiffness, aching, activity sensitivity)
- Overuse irritation (tendons and surrounding soft tissue getting cranky)
However, it’s not a substitute for loading strategies. For example, if your knee pain comes from doing 20,000 steps a day in worn-out shoes, this may help you feel better, but you’ll keep poking the bear.
For a bit of bigger-picture context, knee osteoarthritis is common worldwide. A widely cited 2020 analysis in Annals of the Rheumatic Diseases reported hundreds of millions affected globally (and burden increasing over time). Source: BMJ/ARD (2020).
Quick summary (so you don’t have to reread everything)
Red light therapy knee pain routines work best when you use the right wavelengths (ideally 660nm + 850nm), dose consistently (10–15 minutes per side), and stick with it for at least 2–4 weeks. And, a decent device should disclose irradiance, cover enough area, and make dosing consistent with a timer. If symptoms spike, or you’ve swelling/locking/instability, get evaluated.



